Case Study
Jean Sheehan, Clinical Nurse Specialist University Hospital Limerick
Helen Meagher, Advanced Nurse Practitioner, University Hospital Limerick
Introduction
This case presentation provides an overview of the holistic and multidisciplinary wound management of a 67 year old lady with an infected Diabetic Foot Ulcer on her 4th toe.
Case Presentation:
A 67 year old patient was admitted on 09/07/2019 with cellulitis secondary to a Diabetic Foot Ulcer on her 4th toe. Wound swab cultured MRSA and the patient was a CPE contact. She was commenced on IV Clindamycin to treat infection.
Past Medical History includes:
Type 2 Diabetes, Peripheral Arterial Disease, Diabetic Retinopathy, Hernia Repair, Myocardial Infarction, Hypertension, Smoker, Congestive Cardiac Failure and Poor Glycaemic Control.
Holistic Management
Following 3 days of treatment, she complained of increasing pain and underwent CT angiogram to assess blood flow to her foot. On 16/07/2019 she went to theatre for left femoral angioplasty and stenting and amputation of 4th left toe. Diabetic foot screening was undertaken by Podiatry. The physiotherapist and podiatrist worked together to provide off-loading footwear and to optimise mobility. The endocrinologist and diabetic clinical nurse specialists reviewed and advised re optimising diabetic control to promote healing. Pain continued to be an issue for the patient and the specialist pain team reviewed to advise on management. On 24/07/2019, a wound infection was diagnosed and IV antibiotics were changed to Vancomycin on the advice of infectious diseases team. The tissue viability clinical nurse specialist (TVN) reviewed on an on-going basis and recommended regular dressings. Following TVN assessment on 30/07/2019 a boggy area was detected on the plantar aspect of the foot, which warranted further debridement and incision and drainage of abscess. Vac™ therapy was commenced post operatively. A blood transfusion was required to replace blood loss post op.
The patient developed further complications with recurrent infection and ischaemia requiring amputation of 3rd and 5th toes. The wound measured 7cm long x 5cm, 2.5cm deep. The wound bed was sloughy, bone was exposed with some granulation tissue to wound bed. The wound was initially managed with Vac™ therapy between and post surgeries.
Initiating Vac Veraflo™
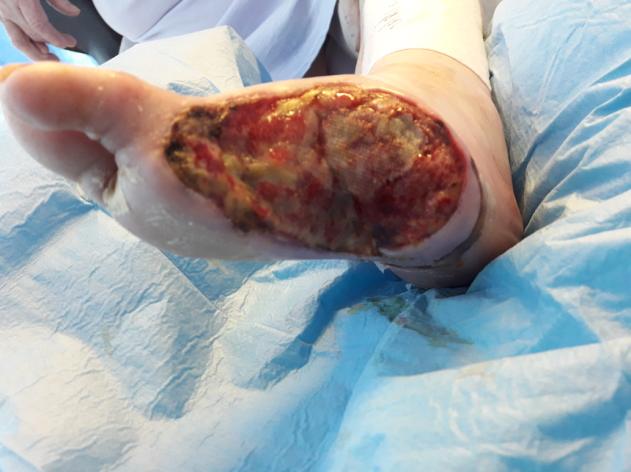
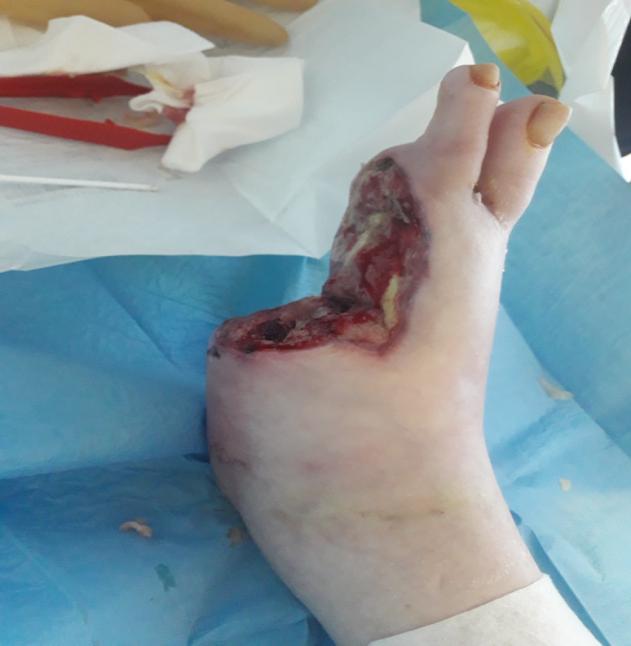
In spite of the treatment outlined above, erythema persisted to the peri wound skin and Veraflo™ was commenced on 28/08/19. Cleanse choice dressing was used with Lavanid 2™ irrigation solution. Wound measured 7cm x 5cm. Wound bed remained sloughy (see figure 1 and 2).
Progress
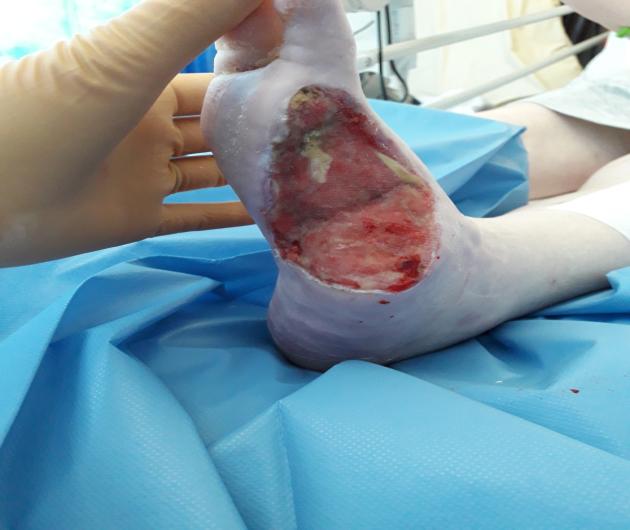
Vac Veraflo™ was continued until 16/09/2019 (Total of 19 days). Wound measurement 6cm x 4cm. Vac™ therapy was recommenced using a bridge granufoam™ dressing at -125mmHg pressure to avoid pressure on the wound or plantar aspect of the foot.
Discharge and follow up
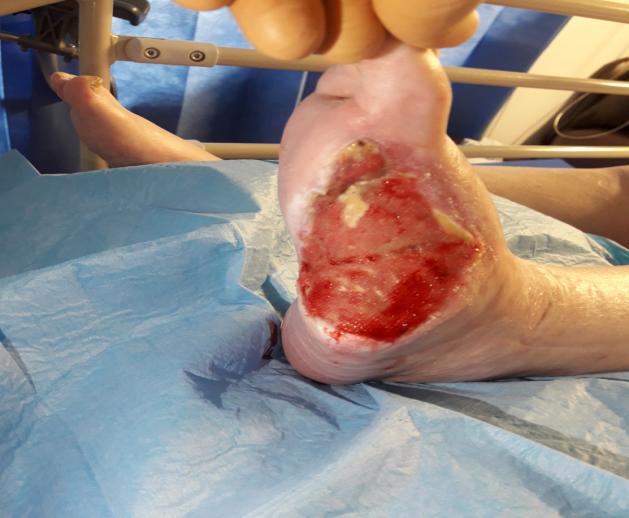
Multidisciplinary treatment in addition to wound care was continued(see figure 4). The patient was referred for rehab prior to discharge home to optimise independence with activities of daily living.
Clinical outcomes/Conclusion
This case study highlights the importance of a Multi-disciplinary approach to the management of wounds. The authors have demonstrated the use of Veraflo™ and Vac™ therapy at the appropriate stages of wound healing. The use of Veraflo™ as demonstrated in the attached photographs, had a positive impact in ongoing debridement and the formation of healthy granulation tissue.
Discussion
This complex case study highlights the importance of a holistic approach to managing a patient with a complex wound. This wound required frequent treatment changes at intervals based on a thorough wound assessment. The Tissue viability CNS played a pivotal role in co-ordinating wound reviews and liaising with members of the multi-disciplinary team to optimise the outcome for the patient.