Case Study
Negative Pressure Wound Therapy with Instillation (NPWTi) in Diabetic Infected Wounds: A Case Report
Institution: SÃO PAULO ANGIOLOGY AND VASCULAR CENTER
City/ Country: São Paulo, Brazil
Leite, Josiane Monteiro; Guimarães, Paulo Celso Motta; Lorena, Maurício; Feitoza, Heidi.
Introduction
Major leg amputations have being the most terrible complication in diabetic patients, vast majority caused by infection and arterial obstruction. In order to obtain success in preserving the limb, it is important a multidisciplinary team working together: plastic, vascular and wound teams. In the last decades diabetic foot ulcer prevalence was 6.3% around the world, but North America had the highest prevalence (13.0%)(1). In the USA, 152 infected wounds per 100 000 hospitalisations are because of diabetic foot ulcers and they are associated with increasing inpatient treatment costs, amputations and mortality(3).
Negative pressure wound therapy combined with timed, cyclical instillation (NPWTi) of topical wound solutions has been recently presented as a new adjunctive modality for treating wounds with signs of infection. Normal saline, antiseptics and antimicrobials all have been proposed in scientific and clinical studies as potentially effective when used with NPWTi for treating heavily infected wounds. We therefore present a case report of usage of negative pressure wound therapy with instillation in a diabeti HB BB hj Hugh to hg nnnnhñ b hg yr ttyt three gggb GF ff FBC tf free uttc infected ulcer. This type of device, might just be the key in reducing amputation incidence within complex infected wounds.
Declaration of Interests
The authors declare that they have no competing financial interests or personal relationships that could have appeared to influence the work reported in this paper.
Case Presentation
A 79- year-old-female patient, diabetic, insulin dependant and with peripheral neuropathy presented with a infected necrotic ulcer of the calcaneus. She was submitted to latin America SEPSE protocol and was classified as severe sepsis. In physical examination and image evaluation (foot Magnetic Resonance and peripheral angiography) were identified: femoro tibial arterial obstruction, diabetic foot ulcer, plantar abscess and osteomyelitis of the calcaneus. Following the removal infected necrotic tissue, she underwent femoro tibial bypass and ABI improved from 0.37 to 1.01.
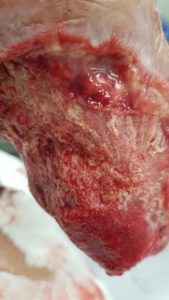
We realize plantar fasciotomy of the foot compartments with drainage and thorough cleaning with saline solution was performed together with debridement of devitalized tissues, and partial resection of the calcaneus. (figures 1).
Since there was extensive exposure of soft tissues , bone and deep structures with a severe local infection we decided to install a negative pressure with instillation to help cleanse the wound and improve infection resolution and healing. The V.A.C. VERAFLO Therapy device was used in this case and we use normal saline only.
The NPWTi system consisted of a reticulated open‐cell foam (V.A.C. VeraFlo™ Dressing; KCI USA, Inc.) that was placed into the wound and sealed with a occlusive dressing. We protected the entire skin around the wound so there was no maceration of healthy tissue.
The first dressing change: During 3 days, NPWTi unit negative pressure was set to 125 mmHg, 20 ml of saline were instilled every hour and soak time set to 1 minute. Subatmospheric continuous pressure of 125 mmHg was applied to all dressing. No topical antiseptic or antibiotics were instilled. We placed the instillation through the upper third of the leg and the aspiration through the lower part of the wound, so the gravity also assisted the process.
On the third day we did the second dressing change: During 4 days 20 ml of saline were instilled every 3 hours and soak time set to 2 minutes. After the seventh day a new dressing change was done with the same device programming for more 4 days. The fifth dressing : During 5 days were instilled 15 ml normal saline every 6 hours and soak time was set to 2 minutes.
NPWTi was discontinued because sufficient granulation coverage free of infection was achieved and the wound were ready for artificial dermal regeneration matrix coverage. An Integra matrix was implanted and then installed standard NPWT with no instillation every 4 days until the twenty-second day (matrix maximum time recommendation), this was followed by skin implants, harvested from the patient’s own thighs (figures 2 and 3) and standard NPWT every 4 days for more 12 days.
Surgical team had no difficulties with V.A.C. VERAFLO Therapy device, as it was considered user friendly to manipulate and install, although all surgical team had training in the procedure beforehand.
We noticed that the patient required less time then traditional dressings to be obtained a granulation coverage free of infection and to became possible the coverage with the dermal regeneration matrix. Rapid infection resolution and wound granulation was observed (16 days), and soon the wounds were ready for artificial dermal regeneration matrix coverage, followed by skin implants.
Consultation follow-up showed good recovery after 1 month with integrity of foot fully recovered (figures 4).
Discussion
Major leg amputations have being the most terrible complication in diabetic patients, vast majority caused by infection and arterial obstruction(2). In order to obtain success in preserving de limb it is important a multidisciplinary team working together: plastic , vascular and wound teams. Wounds with acute infection are still difficult to control and the adjunctive use of NPWTi‐d, rather than standard NPWT, may help manage bacterial bioburden through the removal of wound exudate that may contain infectious materials and potential detrimental inflammatory factor.(4)
Goss et al (5) developed a study whose purpose was to determine the difference in wound bed preparation, with regard to bacterial bioburden, using surgical debridement in combination with NPWTi versus standard NPWT. This study was able to demonstrate that surgical wound debridement followed by one week of NPWTi resulted in a significantly decreased wound bioburden as compared to wound debridement followed by one week of standard NPWT.
Kim et al(6) in a retrospective, historical‐cohort controlled study conducted, with 142 patients requiring hospitalisation for acutely infected wounds demonstrated that a increase in the proportion of closed/covered wounds significantly different between the NPWTi‐d groups versus the standard NPWT group (94% versus 64%, respectively; P = 0·0004). In this case described we presented we are able to notice an acceleration of the wound granulation. Three dressings were performed every four days getting a bone-coated granulation and even having exposed. NPTWti with VACVERAFLO promoted a granulation in 12 days, it occurred rapidly if compared to average wound healing obtained with standard vacuum therapy (30 days).
Brinket et al (6)realized in a prospective clinical study of 131 treated with NPWTi using saline. Results were favourable in 98% of the cases, the wounds could be closed after debridement and following the use of NPWTi. Mean duration of NPWTi was 12·19 days. In this case report we obtained similar results. presented and another relevant fact noted was the the importance of NPTWi for a contamination-free healing obtained.
Conclusion
V.A.C. VERAFLO Therapy was more effective in abbreviate healing in an infected diabetic complex wound than the effectivity with standard vacuum therapy or other conventional therapies. This device was considered safe, user friendly and patient comfortable by the surgical team, who noticed improvement in terms of skin sepsis control, wound granulation and time for “granulation free of infection” when compared to similar cases where other techniques where used.
References
1-Zhang P1, Lu J1, Jing Y1, Tang S1, Zhu . Ann Med. 2017 Mar;49(2):106-116. . Global epidemiology of diabetic foot ulceration: a systematic review and meta-analysis †.
2-Masaki Fujioka. A Retrospective Analysis of Amputation Risk Due to Diabetic Foot and Angioplasty and Free Flap Transfer to Reduce Major Amputation. Intech Open 07\01\2019 : 88351 July 31st 2019
3-Hicks CW, Selvarajah S, Mathioudakis N, Perler BA, Freischlag JA, Black JH III, Abularrage CJ. Trends and determinants of costs associated with the inpatient care of diabetic foot ulcers. J Vasc Surg 2014; 60: 1274– 354.
4-Anghel, EL.; Kim, PJ; Attinger, CE. A solution for complex wounds: the evidence for negative pressure wound therapy with instillation. Int Wound J. 2016 Sep;13 Suppl 3:19-24.
5-S.G. Goss,Negative Pressure Wound Therapy With Instillation (NPWTi) Better Reduces Post-debridement Bioburden in Chronically Infected Lower Extremity Wounds Than NPWT Alone MD, J.A. Schwartz, MD, F. Facchin, MD, J Am Coll Clin Wound Spec. 2012 Dec; 4(4): 74–80.
6-Kim PJ, Attinger CE, Steinberg JS, Evans KK, Hung RW, Smith JR, Rocha ZM, Lavery L. The impact of negative-pressure wound therapy with instillation compared with standard negative-pressure wound therapy: a retrospective, historical, cohort, controlled study. Plast Recontr. Surgery 2014; 133: 709- 16.
Figures
Figures 1 – Inicial treatment with Negative Pressure Therapy


Figures 2 – Granulation of wound achieved with Negative Pressure Therapy
Figures 3 – Usage of artificial skin implants and skin implants


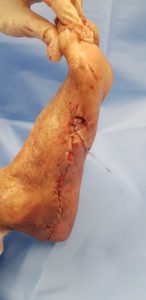
Figure 4 – 4 Months after Infection in consultation
