Case Study
Tiago Henrique Costa
TREATMENT OF MYASIS INFESTATION WITH NEGATIVE PRESSURE WOUND THERAPY WITH INSTILLATION AND A DWELL TIME.
ABSTRACT: Human myiasis is a common condition on our tropical environment, mostly related to pre-existing diseases and poor hygiene habits. Treatment protocols are poorly described, as are the specific advantages of some approaches. Partly because treatment mostly focuses on the underlying pathology. This case demonstrates the incidence of myiasis in a patient with bullous pemphigoid and its management using the classic debridement treatment and one to one larvae removal associated with a 7-day period of negative pressure wound therapy with instillation and a dwell time. Our goal is to demonstrate a new adjuvant therapy to surgery for treatment of this high morbidity pathology, proposing a shorter hospital stay, fewer surgical revisions and less wound manipulation.
INTRODUCTION
Human myiasis is a classically tropical disease caused by dipterous larvae. Its classic clinical presentations are furunculoid myiasis, migratory myiasis and wound or secondary myiasis5. Furunculoid myiasis is characterized by appearance in healthy humans, endemic in rural areas and woods, commonly caused by flies of the species Dermatobia hominis, Cochliomyia hominivorax and Oestrus ovis4. Migratory myiasis, more commonly caused by Gasterophilus intestinalis and Hypoderma spp, larvae of equine and cattle flies, these are more common in Europe and Africa.
Wounds myiasis or secondary myiasis usually occurs in necrotic tissue wounds, with multiple larvae, being associated with Sacophaga, Lucilia and Callitroga4 flies, having as risk factors the presence of open wound, advanced age, low socioeconomic level, poor personal hygiene habits, alcoholism, neoplastic disease, diabetes, psychiatric disorders and compromised immune system5,6. Wound myiasis is particularly challenging to treat as it involves the control of social conditions, underlying pathology, and many times necessity of surgical procedure for debridement of devitalized tissue and mechanical removal of myiasis. This treatment is often time consuming, due to antibiotic therapy for secondary infections, with more than one surgical procedure often required. More recently we have received in the arsenal of complex wound care the use of negative pressure wound therapy with instillation and a dwell time – V.A.C. VeraFlo ™ Therapy, † V.A.C.® Therapy (KCI, an Acelity company, San Antonio, TX).
Such treatment is most appropriate for wounds afflicting patients with multiple comorbidities, complex wounds, with invasive infection, biofilm, patients with ASA (American Society of Anesthesiology Classification) classification greater than 2 especially diabetic and immunosuppressed8. In this report we demonstrate the application of this therapy to an oncologic 89-year-old patient suffering from cutaneous myiasis infestation secondary to a bullous pemphigoid as an adjuvant to classic drug treatment, surgical debridement and mechanical removal of larvae, as well as its rapid clinical course and extinction of the infestation.
METHODS
Male, 89 years old, high blood pressure patient, with anal squamous cell carcinoma who recently underwent treatment with radiotherapy. Was afflicted by a bullous pemphigoid dermatosis. He was admitted due to impetiginization of those lesions, with extensive areas of tissue necrosis and secondary myiasis infestation.
On clinical examination, the patient was lucid, normotensive, normocardial and afebrile.
On examination of the integument, the presence of multiple blisters and pustules at various stages, areas of tissue necrosis focally affecting the skin at full thickness, at points with involvement of the fasciae and musculature, notably in the left upper limb, lateral and anterior face of the distal arm and proximal forearm and hand (Fig.1).
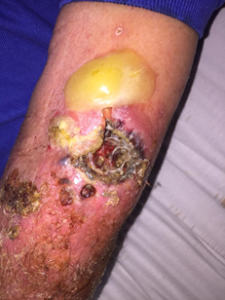
FIG 1: Lateral left distal arm and forearm. Aspect prior to surgical
After initial clinical evaluation and overall treating measures, the specific treatment was proposed by a multidisciplinary team, consisting of intravenous Linezolid antibiotic therapy, oral antiparasitic drug Ivermectin dose 200 μg / kg, and surgical procedure for debridement and larvae removal.
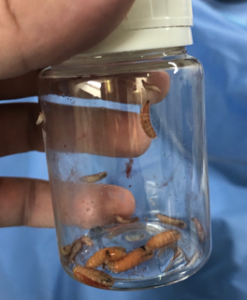
Fig. 2: Larva samples removed surgically.
The surgical procedure was performed under general anesthesia, with devitalized tissue debridement and removal of more than 50 larvae in the entire left upper limb (Fig.2). The infestation was more concentrated in the lateral area of the cubital fossa, region where the necrosis was extended until fascial plane, but without dissection of these spaces. On the left hand at the 2nd interdigital space, necrosis extended to deep planes, compromising deep fascial compartments, with multiple larvae being removed, but tunneling of the lesion made it difficult to fully explore and certify total removal (Fig. 3).
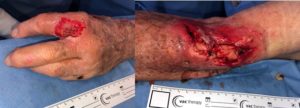
Fig. 3: Left hand and lateral face of the left arm/forearm after debridement and larvae removal
At this point, the option was for negative pressure wound therapy with instillation and a dwell time – V.A.C UltaTM – V.A.C. VeraFlo ™ Therapy (KCI, Acelity Company, San Antonio, TX). The material used was as followed: a large two-part splited V.A.C. VeraFloTM Foam with V.A.C. VeraT.R.A.C. DuoTM. The intact skin adjacente to the wound was covered for its protection with hydrocolloid plates, leaving only the open wound areas in contact with the foam. One of the foam plates was fenestrated creating space for possible larvae to be collected and the second intact plate placed over the first one (Fig. 4), a continuous plate, connecting to the hand and arm wounds (deeper) and several injuries of partial thickness on all posterior forearm face. The V.A.C. VeraT.R.A.C. DuoTM was placed apart, the efferent end proximally, and the afferent distally.
The solution of choice for instillation was 0.9% NaCl saline, with a total volume of 65 ml; This volume was chosen with the help of the V.A.C. UltaTM filling assistant. This was the amount of saline required to return the foam size to the one previous the negative pressure application. The cycle time was 10 minutes of soaking and 4 hours of negative pressure therapy, and the therapy was maintained for 7 days.

Fig. 4: Bottom foam fenestration (wound contact) maintaining intact top foam.
The removal of the foam was performed as a bedside procedure under usual analgesia. Upon removal, the foam was intact, with no purulent or fetid exudates, but with many spurs. Granulation tissue was abundant in the forearm and arm (Fig. 5) and the lesion in the interdigital space was closed with two desiccated larvae at its edge (Fig. 6).

Fig. 5: Immediate aspect following removal of V.A.C. UltaTM

Lesion obliterated after 7 days of V.A.C UltaTM
with 2 desiccated larvae at wound bed.
Fig. 6: Lesion obliterated after 7 days of V.A.C UltaTM
with 2 desiccated larvae at wound bed.
After this period the dressings were performed with ADAPTIC ™ Non-adherent Mesh (Systagenix, an Acelity company) being changed every 2 days, with epithelium regeneration occurring rapidly to the 14th day of follow-up.

Appearance after 14 days, showing advanced epithelial regeneration
Fig. 7: Appearance after 14 days, showing advanced epithelial regeneration.
Patient remained hospitalized due to new sparse pemphigoid lesions for analgesia and local care and was discharged after 28 days of hospitalization, without the need for a second surgical procedure and without dressings (Fig. 8)
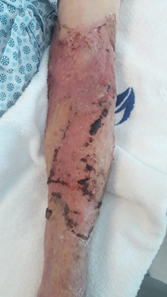
Fig. 8: Appearance at discharge.
DISCUSSION.
The occurrence of myiasis in this patient shows the epidemiological standards described in the literature4,5,6: elderly patient with dermatoses, neoplasia and low hygienic conditions.
Standard treatment: debridement, oral antiparasitic, mechanical larval removal and antibiotic therapy to control secondary infections was instituted. Notwithstanding these negative pressure wound therapy with instillation and a dwell time – V.A.C UltaTM has been applied as adjuvante ccording to current indications, wound care in a patient with complex wound, elderly, with multiple comorbidities and gross pre-debridement contamination1,3,7,8,9.
The application of the cyclic soaking solution alterned with the subatmospheric therapy was in our view one of the major factors that allowed the use of closed dressing for 7 days without formation of collections. Only 1 surgical procedure was required during the entire hospitalization, and no need to manipulate the wound within 7 days of debridement, which generated comfort for the patient and his family. The therapy was also effective in depriving the larvae of oxygen, attracting them to the edges of the wound and subatmospheric pressure desiccating them, avoiding local decay. Granulation tissue obtained after 7 days drew attention to an 89-year-old patient with active dermatosis and an almost complete epithelial regeneration was noted after 14 days.
CONCLUSION
Negative pressure wound therapy with instillation and a dwell time is a treatment modality that has gained ground in the practice of treating complex wounds, especially in the presence of comorbidities, advanced age, and other epidemiological characteristics that predicts wound healling problems. In this case, the length of stay was not prolonged by the treatment of myiasis and tissue necrosis. In addition, the need for further exploration of the wound for myiasis removal was eliminated and the initial surgical time was greatly reduced.
.
An important fact to be described was the lack of need for dressing changes during the infestation phase outside the operating room, providing greater peace of mind and comfort to the nursing staff, and the absence of visual contact between the patient and family members with larvae, thus avoiding greater emotional wear..
Thus, we present a potentially serious and of laborous treatment pathology effectively and quickly managed with the aid of negative pressure wound therapy with instillation and a dwell time.
REFERENCES:
- Omar, M. Gathen, E. Liodakis, E.M. Suero, C. Krettek, C. Zeckey, and M Petri. A comparative study of negative pressure wound therapy with and without instillation of saline on wound healing. Journal of Wound Care 2016 25:8, 475-47
- Semsarzadeh NN, Tadisina KK, Maddox J, et al. Closed incision negative-pressure therapy is associated with decreased surgical-site infections: a meta-analysis. Plast Reconstr Surg. 2015; 136:592602.
- Back DA, Scheuermann-Poley C, Willy C. Recommendations on negative pressure wound therapy with instillation and antimicrobial solutions – when, where and how to use: what does the evidence show?. Int Wound J. 2013 Dec;10 Suppl 1:32-42.
- Cilla G, Picó F, Peris A, et al. Miiasis genital humana por Sarcophaga. Rev Clin Esp 1992; 190:189-90.
- McGraw T.A., Turiansky G.W. Cutaneous myiasis.J Am Acad Dermatol. 2008;58(6):907–926.
- Marquez AT Mattos MS Nascimento SB . 2007. Miíases associadas com alguns fatores sócio-econômicos em cinco áreas urbanas do Estado do Rio de Janeiro. Revista da Sociedade Brasileira de Medicina Tropical 2007 40(2): 175-180.
- Huang C, Leavitt T, Bayer LR, Orgill DP. Effect of negative pressure wound therapy on wound healing. Curr Probl Surg. 2014;51(7):301-331.
- Kim PJ, Attinger CE, Olawoye O, et al: Negative-pressure wound therapy with instillation: international consensus guidelines. Plast Reconstr Surg 2013;132:1569-1579.
- Kramer A., Dissemond J., Kim S., Willy C., Mayer D., Papke R., Tuchmann F., Assadian O., 2017. Consensus on Wound Antisepsis: Update 2018. Skin Pharmacology and Physiology, 31(1):28-58.