Case Study
Abstract
This case study present a patient with an Unstageable Pressure Injury where surgical debridement was not an option as patient was considered too ill. NPWTi using Cleanse Choice dressings demonstrated a positive result that facilitated softening and removal of thick eschar. The instillation therapy also reduced the inflammatory makers at the wound bed and improved patient outcome.
Introduction
Pressure injuries (PI) are debilitating and painful that are considered mostly avoidable and a number of well published international guide
lines provides strategies to reduce these incidences. Identifying early stages of tissue injury using the National Pressure Ulcer Advisory Panel (NPUAP) guideline and European Pressure Ulcer Advisory Panal (EPUAP), will guide clinicians to provide relief of person suffering from or at risk of pressure injury 5,6
Standard pressure injury management includes identifying those who are at risk, performing regular skin assessment, providing equipment to redistribute pressure, regular repositioning, managing microclimate and providing adequate nutrition.
However, despite these guidelines and preventative strategies, pressure injury still occurs specifically in those who are elderly and vulnerable. Two thirds of the incidences occur in the elderly above 70 years of age and the prevalence of pressure injuries in hospital is reported to be close to 5% in one study on India. 1.
Pressure injuries are defined as tissue damaged as a result of prolonged pressure usually over boney prominences. Shearing, friction and an increase in microclimate can also contribute to altering skin integrity and increase the risk of developing pressure injury. 2.
Staging of PIs help clinicians classify the depth of tissue damage. Stage 1 is intact skin with non-blanching redness. Stage 2 involves the epidermal skin loss with an open wound that is shallow with or without slough. Stage 3 is full thickness tissue loss, where bone or tendon may or may not be visible. Stage 4 is full thickness tissue loss with exposed bone, tendon or muscle. Suspected deep tissue injury is defined as dark marooned intact skin that maybe blood-filled that could evolve to be superficial or full thickness tissue loss. PIs with dry thick eschar or thick slough is categorised as Unstageable due to unknown depth of tissue damage, until the eschar and or slough is removed.2.
This case study presents how the use of Negative Pressure wound therapy with instillation using Cleanse ChoiceTM dressing, assists with the removal of thick slough from a sacral PI that was categorised as Unstageable.
Negative Pressure wound therapy (NPWT) with instillation (NPWTi) or V.A.C VerafloTM therapy is unique in that is uses specifically designed dressing that allows instillation of wound solution with NPWT. The dressing is less hydrophobic that assist with fluid distribution and removal of fluid from the wound bed. Using Cleanse Choice foam dressing will further facilitate removal of thick wound exudate, slough and infectious material. The contact layer with 1 cm holes provide mechanical movement at the wound bed and breaking down the thick slough, whist the 2 cover layers without holes assists with filling the various wound depth and capturing large volume of fluid before entering into the tubing.3.
Norman (a pseudonym) is a 90 year old male who was admitted via emergency department from home post fall. He also had community acquired pneumonia and cellulitis of lower limbs. Pre fall, Norman was living with his wife and independent with activities of daily living. He quickly became deconditioned due to complications with acquiring aspiration pneumonia and newly diagnosed Ca of Prostate. His medical history included Congestive Cardiac failure, Atrial Fibrillation and bilateral inguinal hernia. . He was monitored closely in intensive care unit and had drainage of pleural effusion. Despite preventive strategiesthat was implemented early, due to doubly incontinent status, deconditioning, immobility and newly diagnosed with Crytococcal Meningitis, he quickly developed Stage 2 pressure injury that deteriorated to thick sloughy, Unstageable, pressure injury at the sacrum. Septic screen was also performed to find the source of increased inflammatory markers, including wound swab, which showed no significant growth. However, CT scan showed he had osteomyelitis and was commenced on intravenous antibiotics and conventional wound dressings were applied with no improvement. It was decided, in consultation with the treating team, to initiate NPWTi to breakdown the thick slough and manage the infection topically.
Methods
NPWTi was initiated using Cleanse Choice TM in conjunction with using super oxidised solution as a choice of wound solution. Twelve mls of solution was instilled with dwell time set at 10 minutes and pressure setting at 125mmHg every 2 hours. Trac disc was place directly over the main wound without bridging to allow direct instillation and removal of wound exudate and solution fluid. Dressings were initially changed every third day. The first 2 dressing changes were applied without complications. However, the alarm indicating instillation blockage kept alarming despite re-application with ‘bridging’ of the foam.
Wound solution volume was adjusted according to wound size as the thick slough started to breakdown and was conservatively debrided.
Cleanse ChoiceTM dressings was used for duration of five weeks and then was switched over to Veraflo Granufoam for 2 weeks.
Wound measurements and photography were taken initially and minimum on a weekly basis.
Results
On day 11, after initiating NPWTi, the thick eschars started to breakdown and soften further to allow conservative debridement to be performed. The original size of the wound was 5.5cmx 3cm but depth of injury was not able to be measured due to thick eschar. (Photo 1). A few applications using Cleanse Choice TM was required due to ‘instillation blockage’ alarming despite troubleshooting the issue. There was evidence that the ‘holey’ layer was in contact with the thick eschar as we could see the shallow holey imprint as seen in photo 2.
Once the eschar softened and started to break down and be debrided, the wound cavity and size measured to be L-7cm x W-4.5cm x D-3cm with undermining. The wound base was covered with 50% sloughy tissues which was difficult to debride with scalpel and scissors due to the depth. (Photo 3,4)
The next few applications using Veralfo Granufoam continued to show slight improvement with wound size reduction (L- 4cm, W- 4cm, D- 1cm), however, the wound remained clean with mostly granulation tissue. (Photo 5, 6)
Discussion
The use of NPWTi with Cleanse Choice TM definitely facilitated a faster result with Eschar breakdown and cleansed the wound compared to conventional dressings. There was established Osteomyelitis from CT scan and the sacral wound swab showed 3+ corynebacteraim striatum, 3+ corynebactim amycolatum and mixed coliforms. Repeated swab showed reduced counts of corynebacteraim striatum but significiant staphaureus.
Extrinsic factors such as patient’s age, wound infection, deconditioning and his ‘unfit’ status for surgical wound debridement would have extended his length of stay. Initiation of NPWTi with Cleanse ChoiceTM and Veraflo Granufoam, despite some unknown issues with “instillation blockage”, still facilitated slough/ eschar breakdown and cleansing of the wound. This was evident in reduction of the wound size and depth which correlated with the reduction of the inflammatory markers. Veraflo Granufoam was ceased and conventional dressings was applied. Currently, this non healing wound has become ‘Stagnant’ and a collagen matrix was applied with the aim to ‘kickstart’ the healing process.
Conclusion
NPWTi with Cleanse Choice TM and Veraflo Granufoam definitely facilitated eschar / slough breakdown and wound cleansing, in particularly in cases where extrinsic factors hindered surgical debridement.
References
- Agrawal.K and Chauhan. N 2012. Pressure ulcers: Back to the basics. Indian Journal of Plastic Surgery May-Aug;45(2); 224-254
- Carville.K 2012 Wound Care Manual 6th Ed. Silver Chain
- Weblink: https://www.acelity.com/healthcare-professionals/history-of-innovation/vac-veraflo-therapy
- Pressure Injury Prevention and management guideline http://slhd-intranet.sswahs.nsw.gov.au/SSWpolicies/pdf/SLHD/SLHD_PD2017_034.pdf
- National Pressure Ulcer Advisory Panel guideline 2014 http://www.internationalguideline.com/downloads
- European Pressure Ulcer Advisory Panel guideline 2014 http://www.epuap.org/wp-content/uploads/2016/10/quick-reference-guide-digital-npuap-epuap-pppia-jan2016.pdf
Photo 1
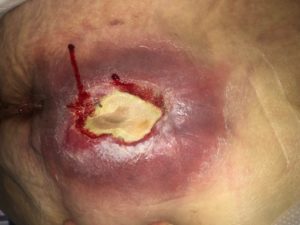
19/9/2019
Photo 2
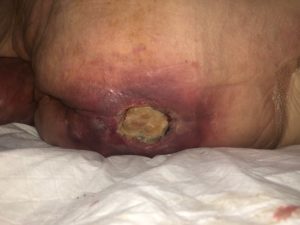
22/8/2019
Photo 3
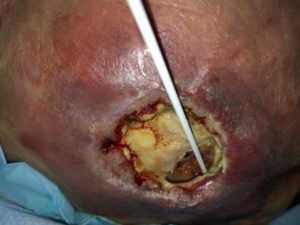
26/8/2019
Photo 4
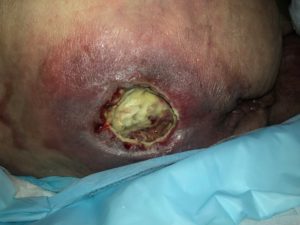
26/8/2019
Photo 5
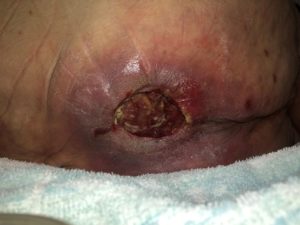
16/9/2019
Photo 6
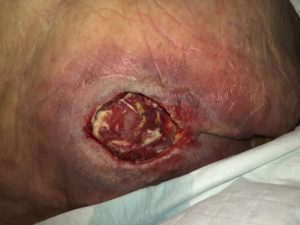
27/9/2019