Case Study
Abstract
Knowledge of pressure injuries (PI), although not always known as pressure injuries, have been with us for a very long time. A Millicent Ashdown in her Complete system of Nursing talks about their symptoms and treatment back in 1917. With the advancement of modern medicine, the number of these injuries in our district have fallen however we are still occasionally seeing severe stage four PI’s most likely due to the acuity of the patients that we are now able to treat. The treatment for these PI’s often require surgery to debride to necrotic tissue as well as close the deficit. This however, is not always a viable option and alternatives need to utilised to help optimize the healing process and reduce healing times.
Patient History
32 year old male presented to Emergency Department on the 4/1/19 with a history of Blistering with Purulence in the lower legs over 3-4 days and then experienced fever, chills, and right thigh pain during the night of presentation.
The initial diagnosis was suspected necrotizing fasciitis, cellulitis with central necrosis, severe peripheral oedema with multiple ulcerations and acute on chronic kidney injury . Soon after presentation he was transferred to ICU due to clinical deterioration.
Medical history includes; Viral Myocarditis in 2016, which resulted in severe dilated Cardiomyopathy, Gout, Obesity, ex-smoker.
During a 34 day ICU stay :
He Required significant Vasopressor and Inotropic support (noradrenaline weaned by the 31/01)
The Acute Kidney Injury on background of Chronic renal impairment necessitated the use of Continuous Renal Replacement Therapy.(CRRT) until the 05/02 when he was transferred to intermittent Haemodialysis.
Also during his stay, he underwent multiple surgeries for lower limb wounds including debridement and washout of right thigh, lower legs and left foot.
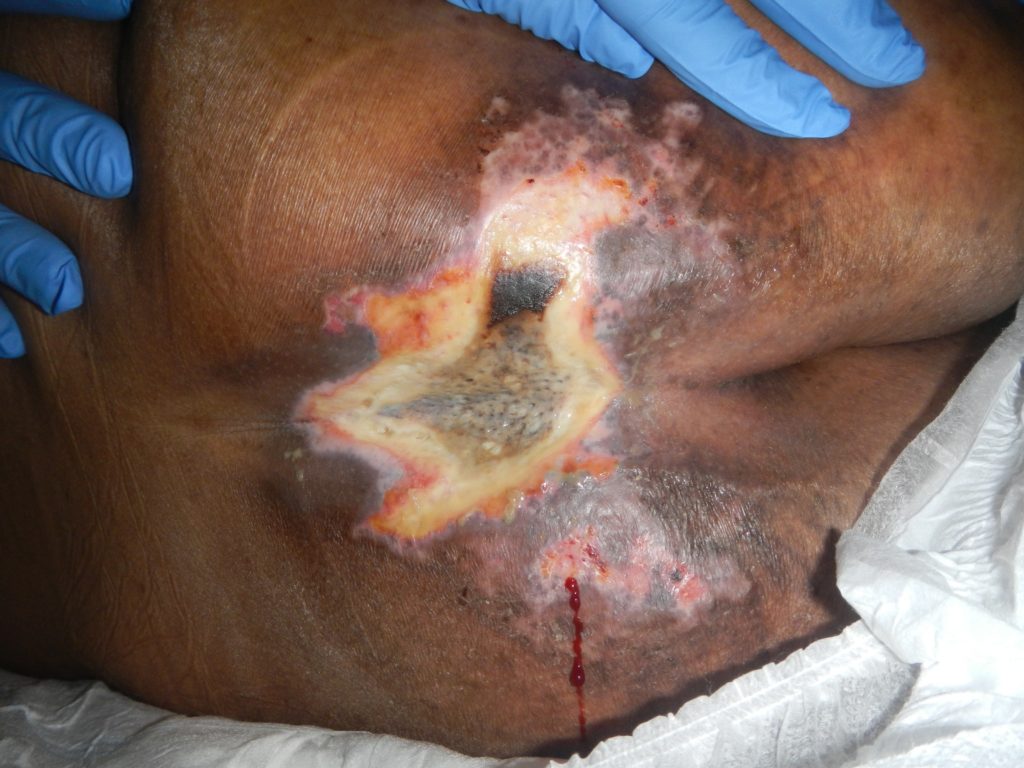
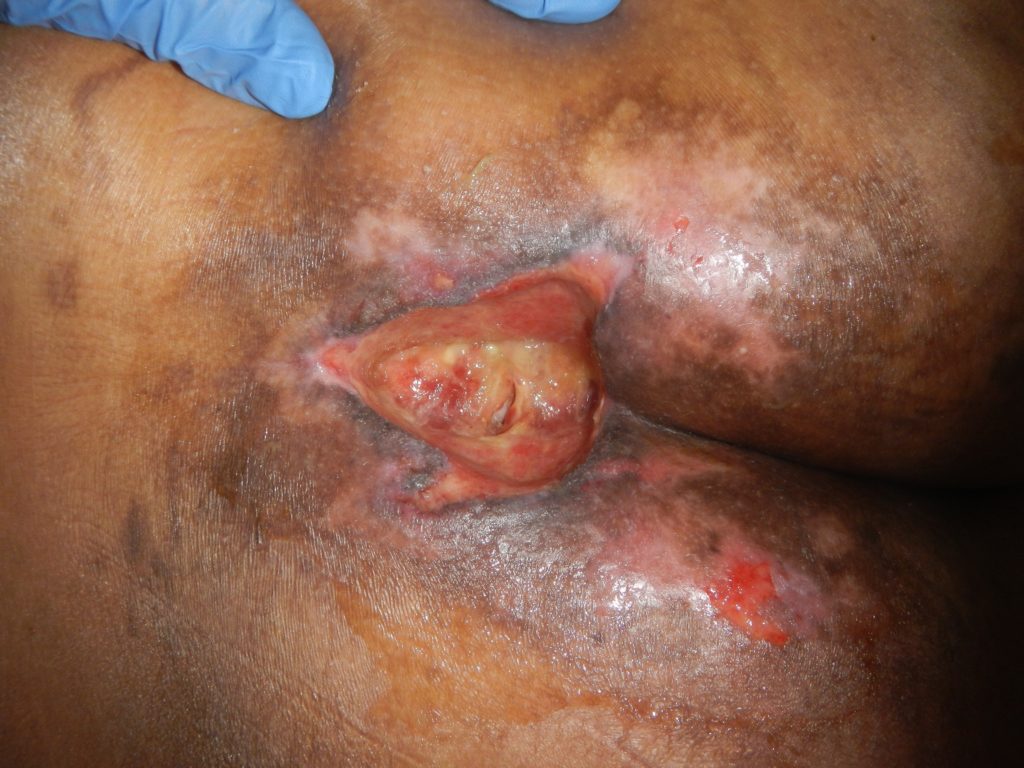
There were two small pressure injuries (PI) on the left buttock which was present on admission and on the 11/2/19 the PI was classified as unstageable with the central area being thick eschar. (Fig 1)
Treatment of the Pressure Injury
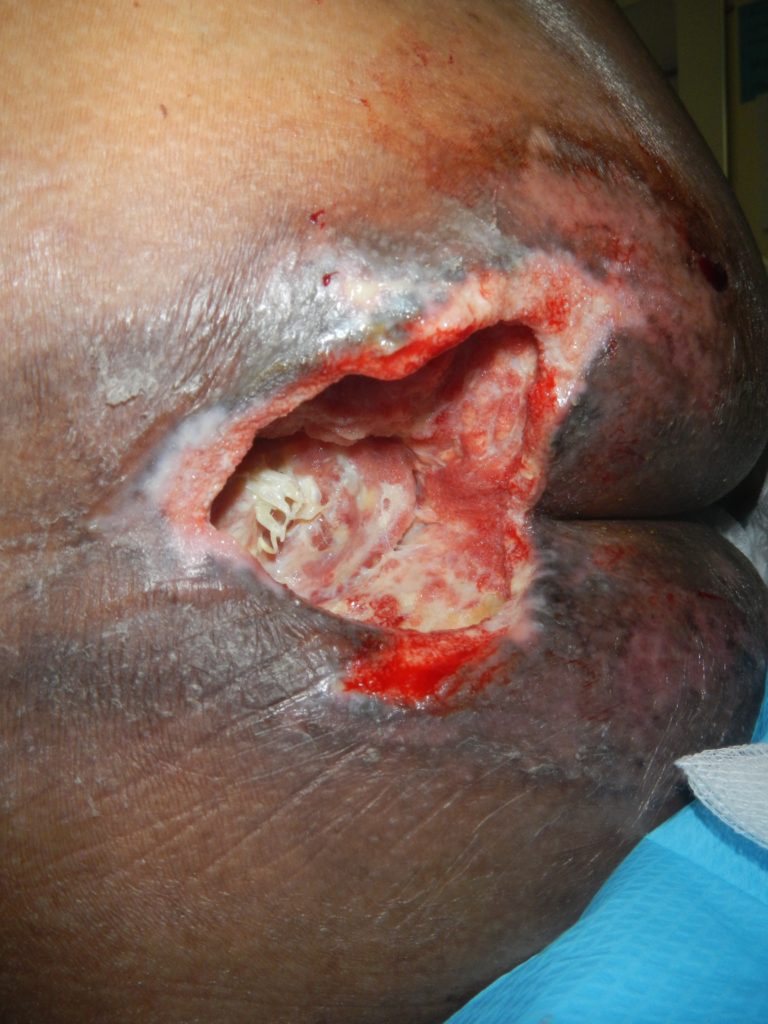
On 25/2/19, the thick eschar of the PI had broken along with some of the necrotised adipose tissue, however, the wound bed and true depth of injury remained hindered due to the remaining thick devitalised tissue, possibly a stage 4 but unable to confirm at that point in time. Devitalised tissue was sharp debrided however; yellow slough remained on 50% of wound bed.
The cavity was approximately 4 – 5cm deep, 7cm length and 5cm width. The wound care plan was to continue dressing with hydrofiber dressing to absorb wound exudate and help with autolysis of the devitalised tissue, and a foam dressing to help with exudate management and offer some redistribution of pressure.
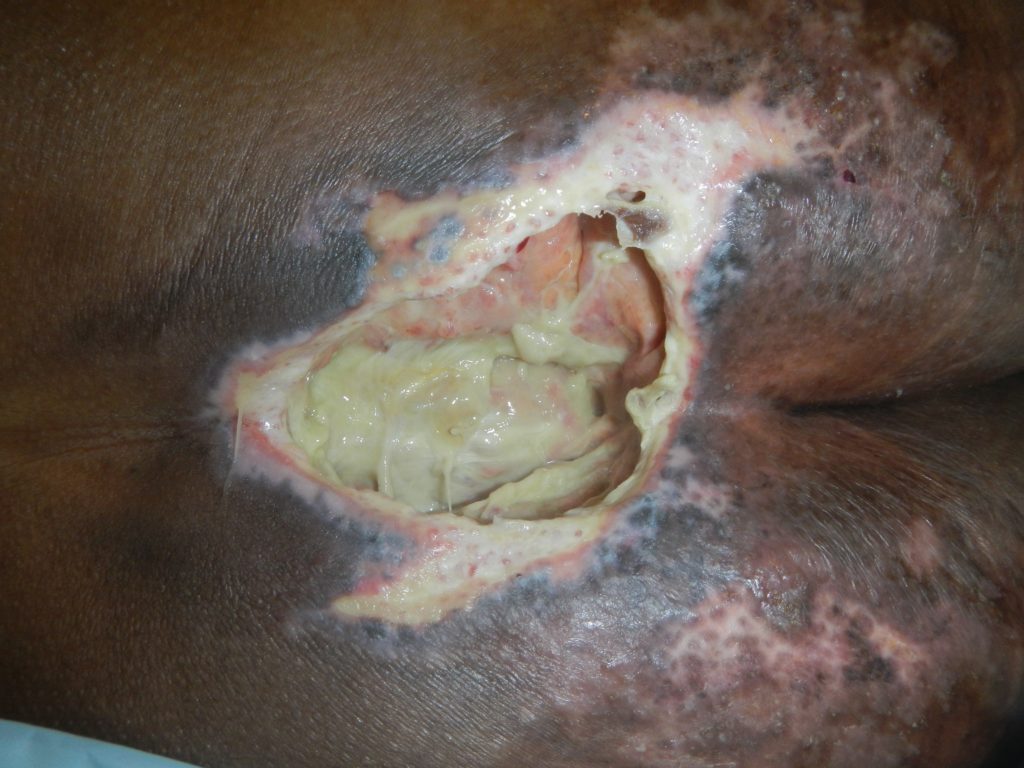
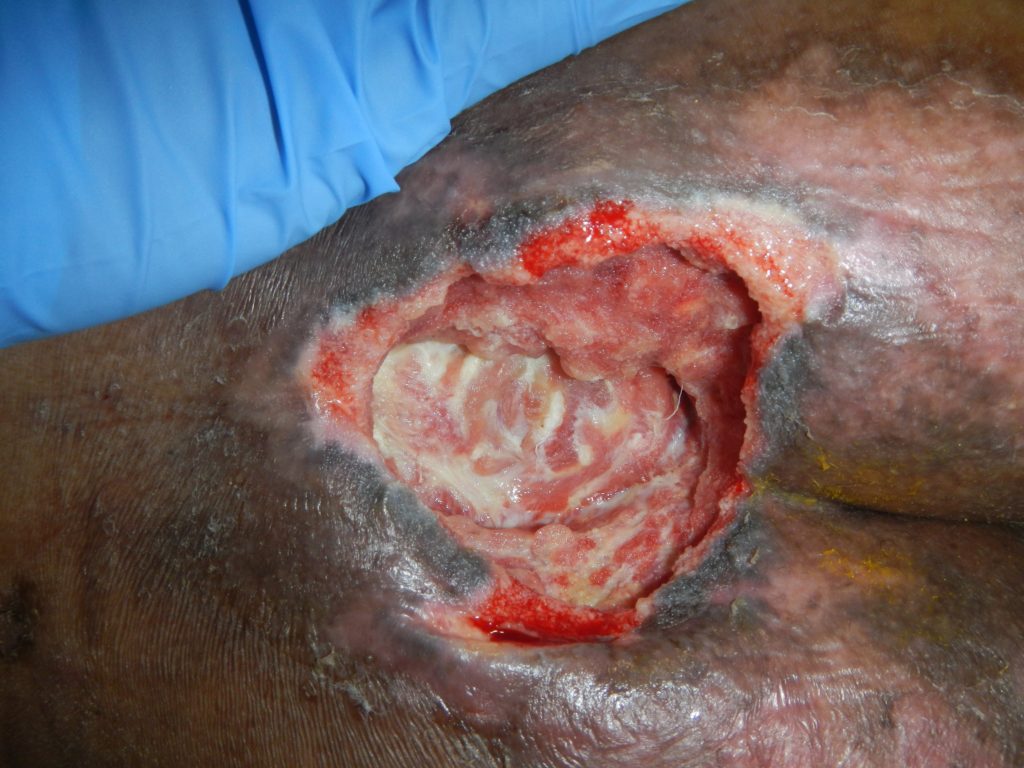
On 27/2/19, the PI was classified as a stage 4 with fascia and muscle visible (Fig. 2). Negative Pressure Wound Therapy with Instillation and dwell (NPWTi-d) was initiated with reticulated open cell foam with through holes- Cleanse Choice (ROCF-CC) to assist in the removal of the remaining devitalised tissue and to promote healing.
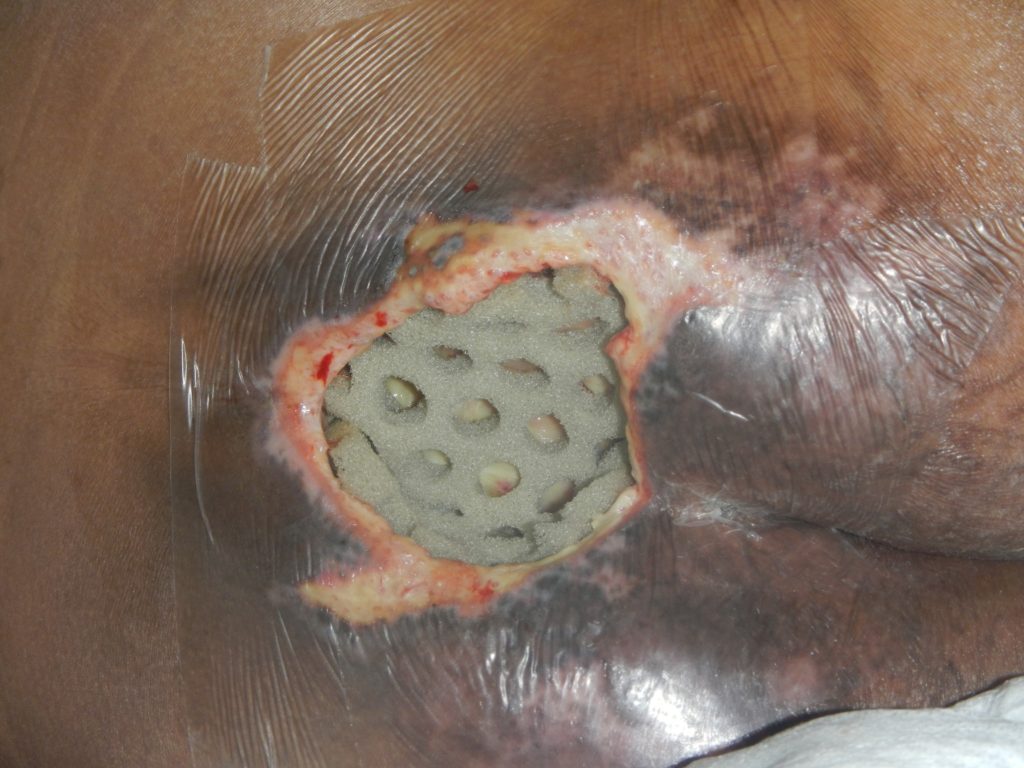
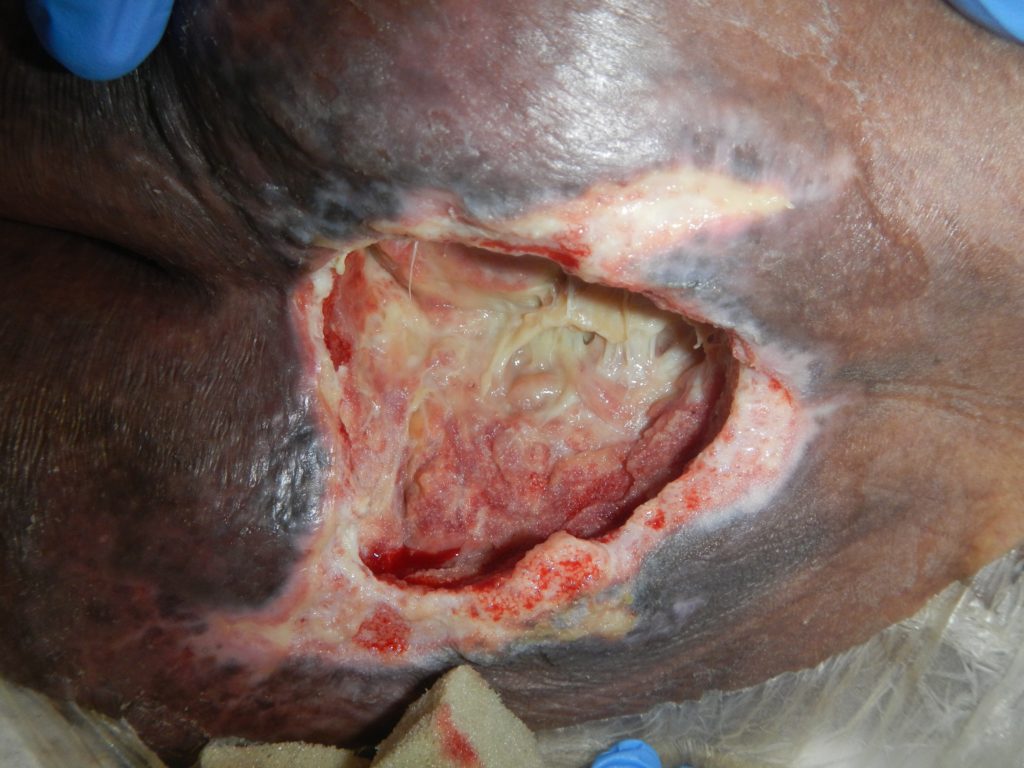
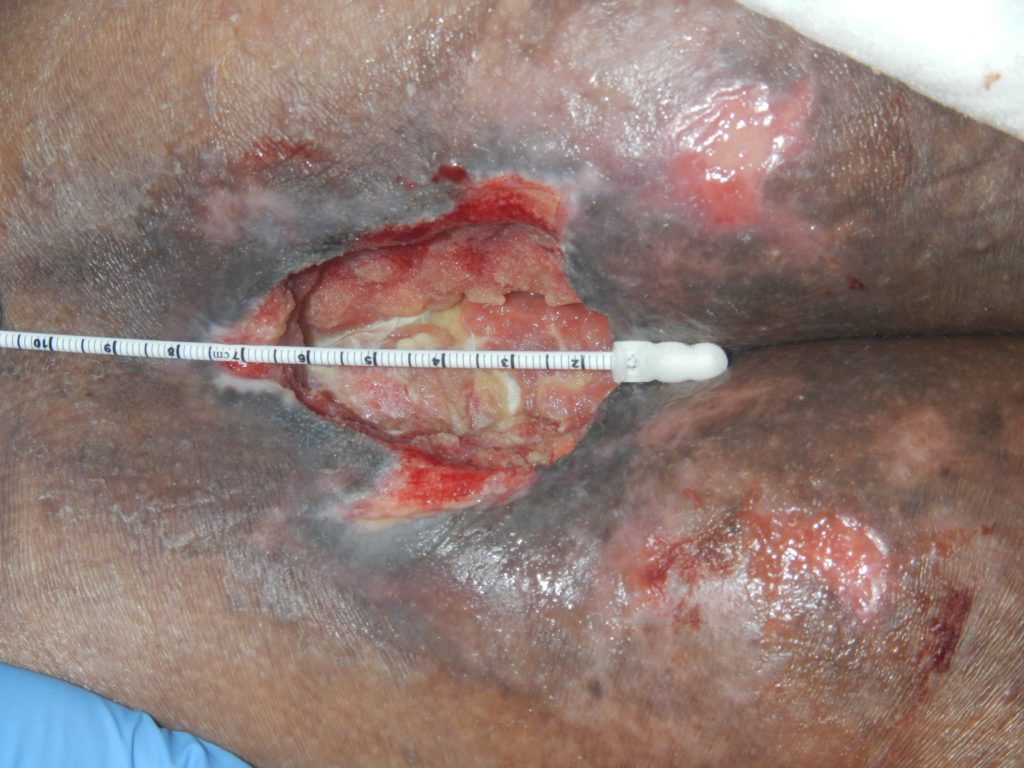
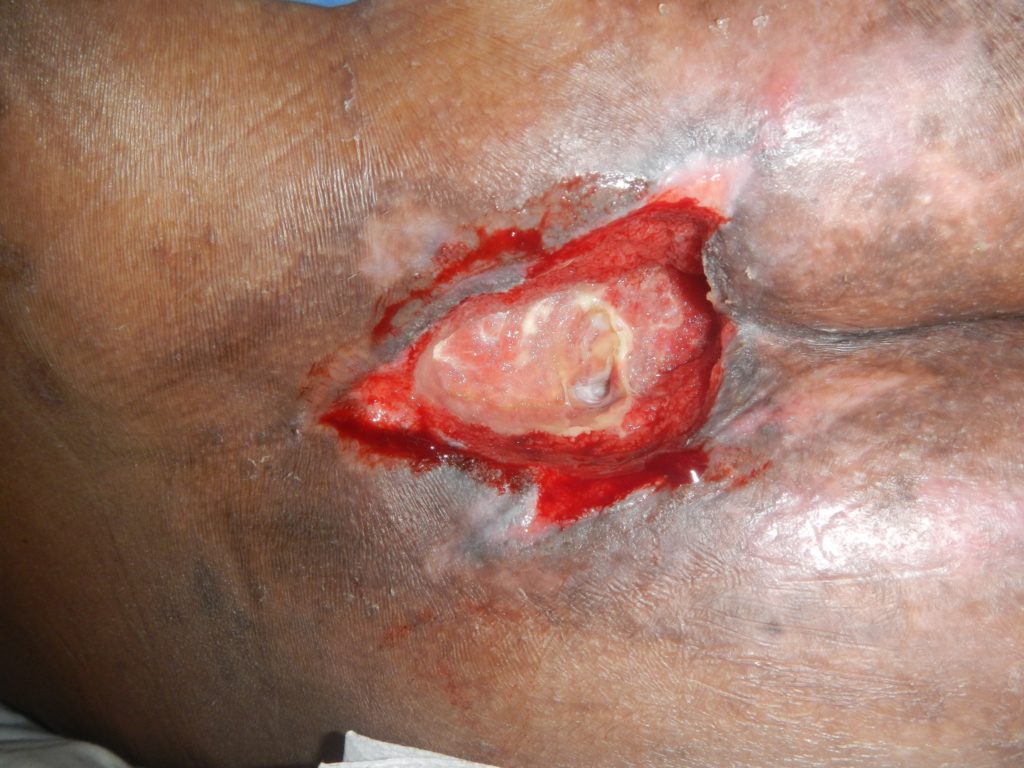
At the first dressing change on the 1/3/19, there was a significant reduction in devitalised tissue and slough (Fig. 3) Continued improvements in the wound bed were seen at the 2nd and 3rd dressing changes along with a reduction in wound size (Fig. 4).
NPWTi-d with ROCF-CC was continued as the wound bed consistently improved with a decrease in devitalised tissue and improvements in granulation tissue (Fig. 5 & 6).
NPWTi-d continued (Fig. 7) until day 50 (Fig. 8).
On the 2/4/19, the patient was stepped down to standard NPWT and discharged to a rehabilitation facility for ongoing care.
Conclusion:
The utilisation of NPWTi-d with ROCF-CC for 34 days with this patient assisted in removing devitalised tissue from the wound bed and promoting new granulation tissue. As this patient was not a candidate for surgical debridement, this treatment gave us another option to progress a complex wound into a more manageable healing wound.
I wish to acknowledge my colleague Ashleigh Dolton and the ward nurses who assisted me with the treatment and management of this patient’s wound.
References:
- A.Millicent Ashdown, (1917) The Complete System of Nursing page 17, Waverley Book Company Ltd
- 2017 NSW Pressure Injury Point Prevalence survey report. http://www.cec.health.nsw.gov.au/__data/assets/pdf_file/0009/435357/2017-NSW-Pressure-Injury-Point-Prevalence-Survey-report.pdfRoyal Prince Alfred Hospital, Camperdown, NSW, Thomas Leong CNC Skin Integrity and Wound Management