Case Study
Introduction
An 86-year-old male had been admitted for an elective second stage hip revision. His medical history consisted of IHD, CCF, TIA, osteoporosis, hypercholesterolemia and hypothyroidism. Surgical history was a previous left total hip replacement complicated by infection and removal of prosthesis. Medications included Cholecalciferol, Rosuvastatin, Levothyroxine Sodium, Paracetamol, Loratadine and Ciprofloxacin.
Patient
He had developed a post-operative infection requiring return to theatre and washout. Post-operatively he became hypotensive requiring vasopressor support which was administered via an intravenous cannula in his left cubital fossa.
Diagnosis
Twenty-four hours post administration he was noted to have erythema, pain, induration, swelling and bullae developing on the medial aspect of his left arm. Initially thought to be necrotising fasciitis, his observations and inflammatory markers remained stable. The Plastic surgeons were consulted and CT conducted which revealed some subcutaneous gas. It was suspected that extravasation was the aetiology of the developing tissue necrosis. He was not a candidate for further theatre therefore the wound management team was consulted to review and develop a plan of care.
Method
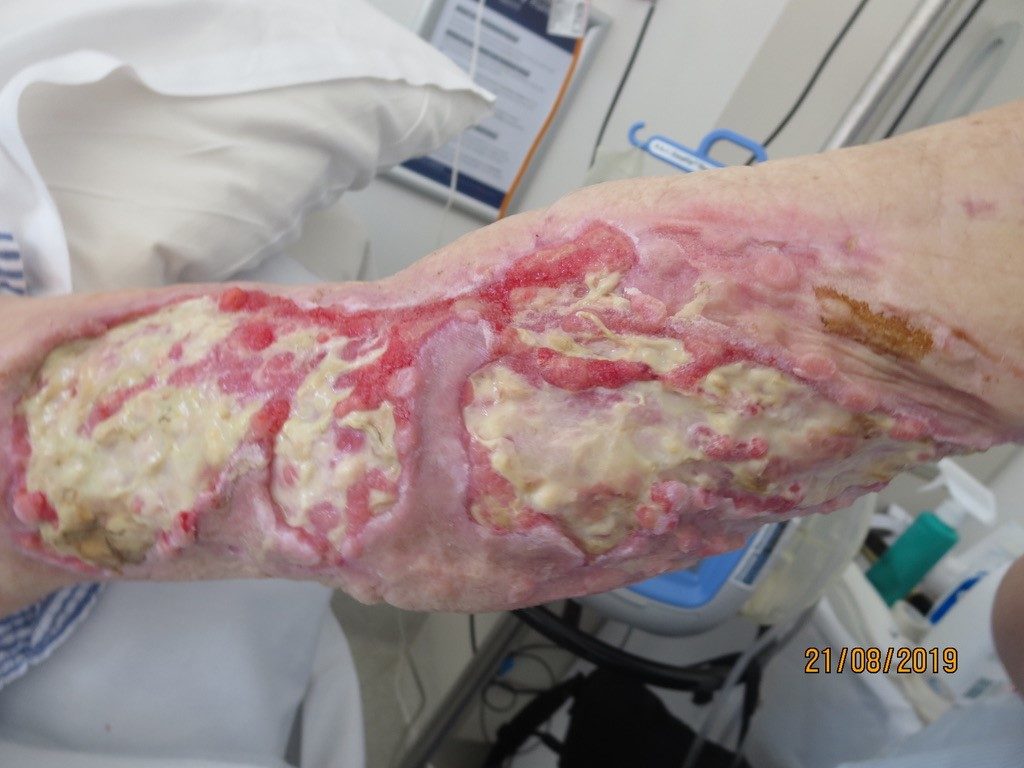
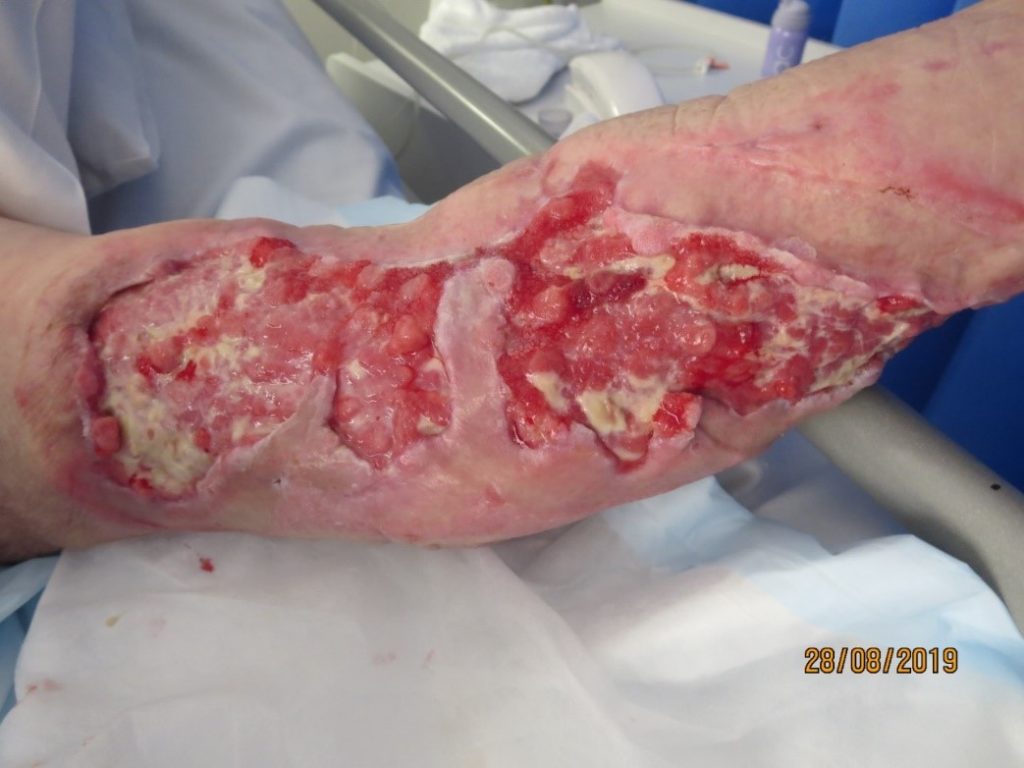
The wound was predominantly eschar and the exuding heavily. The goal of care was to promote autolytic debridement, provide microbial cover for the bioburden and manage exudate. A silver interface was selected as the primary dressing, a super absorbent pad as the secondary and secured with simple crepe bandage; changed on a daily basis. The current plan in conjunction with bedside conservative sharp wound debridement, was gradually autolysing the necrotic tissue and there was evidence of demarcation (Figure 1. and Figure 2). However, there was ongoing concern that if the arm wound became infected, this placed great risk of him developing further infection in the left hip joint.
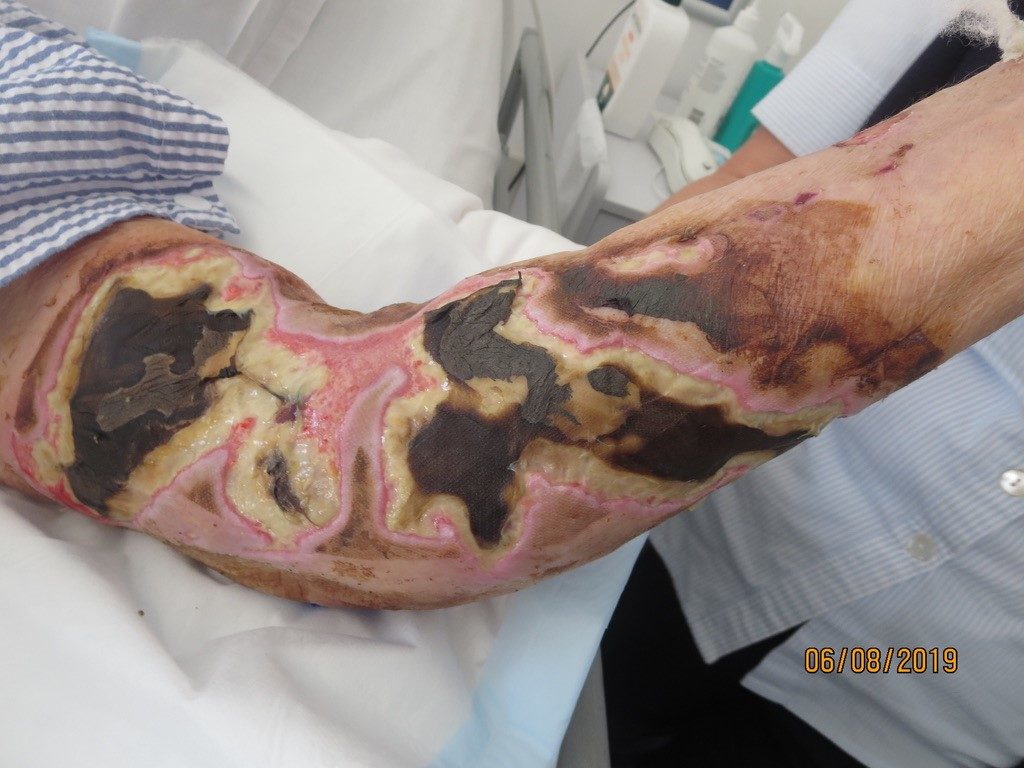
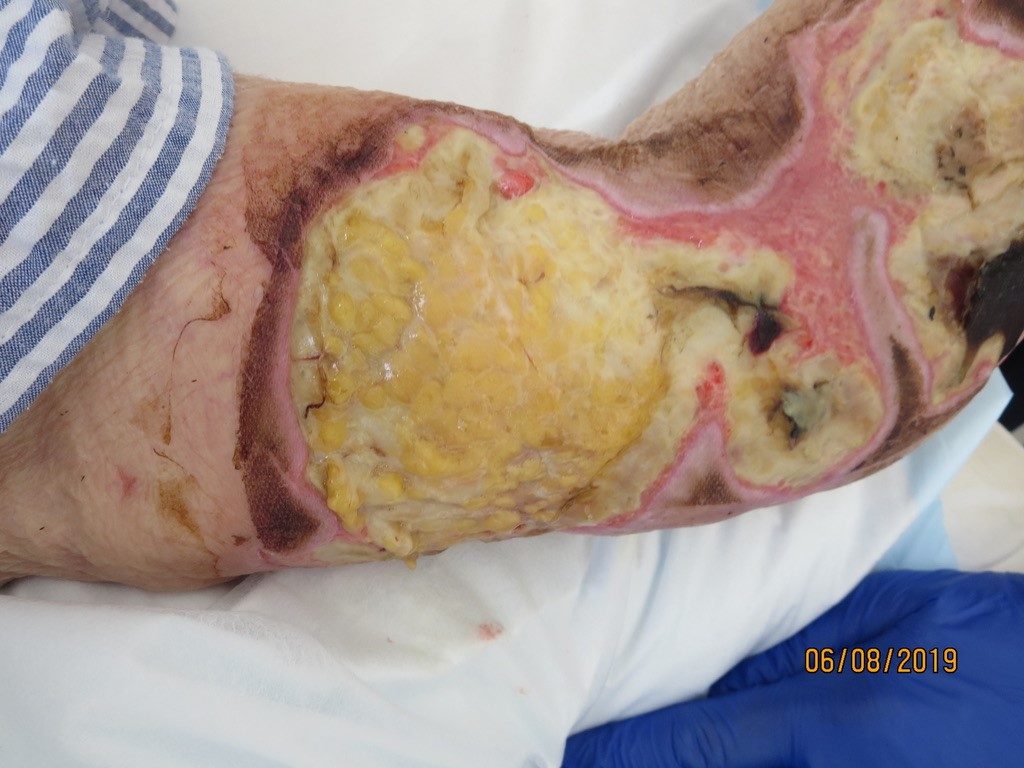
Results
The decision was made to commence Negative Pressure Wound Therapy with Instillation and Dwell (NPWTi-d). This would allow for gentle yet sustained debridement, reduction of bioburden, promotion of granulation tissue and wound contraction. This would also reduce need for frequent dressing changes and efficiently manage wound exudate. The use of the reticulated open cell foam dressing with through holes, Cleanse Choice was selected to facilitate the drainage of viscous exudate and slough and facilitate the stimulation of granulation tissue. The wound was bordered with cohesive seal to protect the peri-wound skin and prevent instillation fluid from leaking (Figure 3). Initially, using the fill-assist function, 85 ml of Normal saline was delivered to the wound bed, allowed a dwell time of 15 minutes then the negative pressure cycle of 3.5hours. Fluid volumes were adjusted as the wound reduced in size.
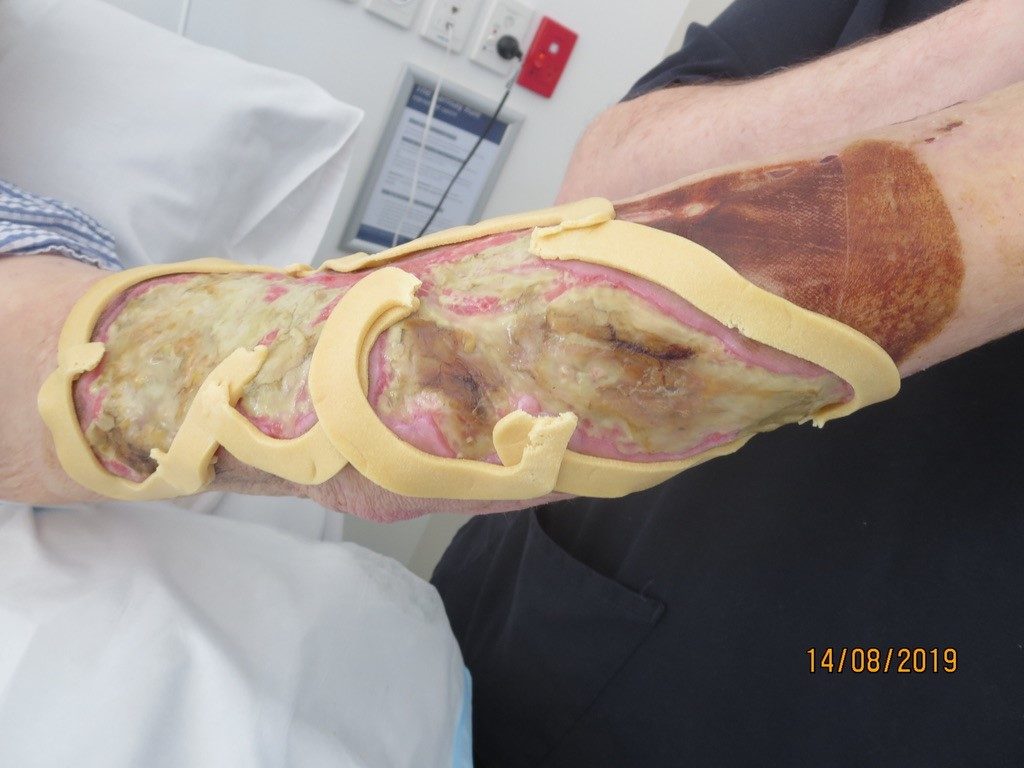
Progress
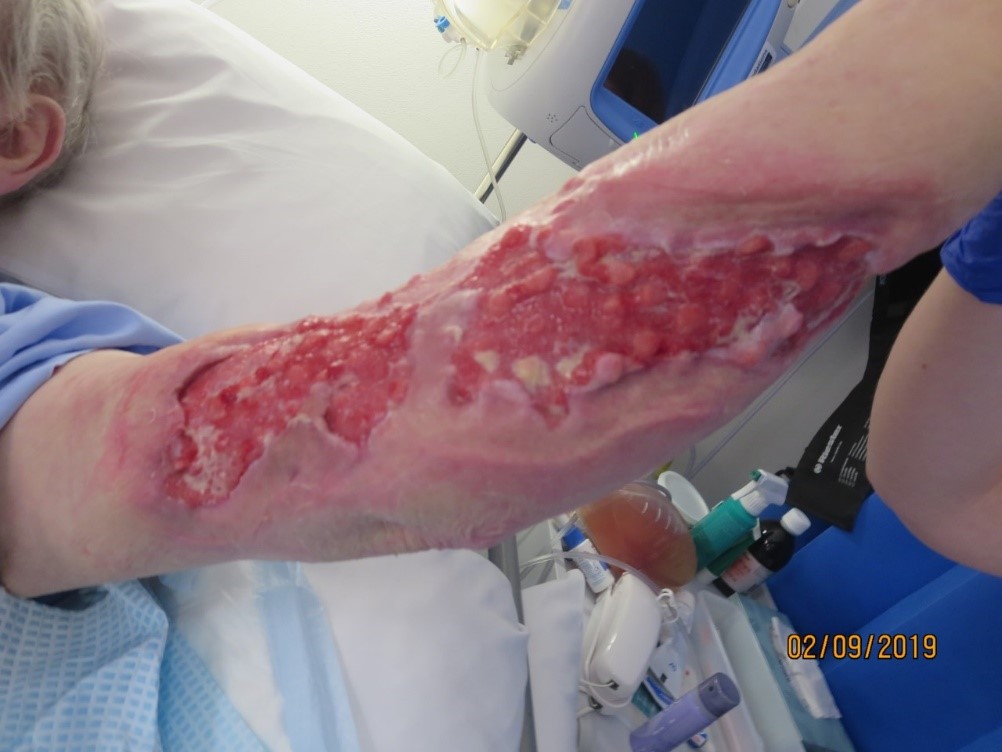
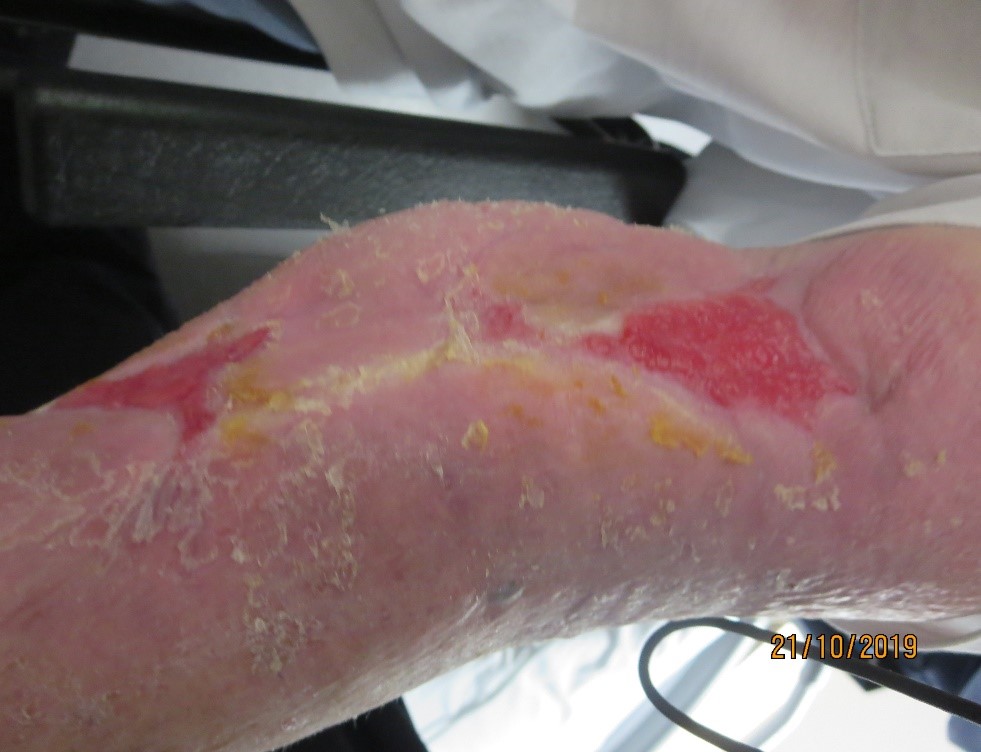
After 72 hours the initial dressing was removed revealing a reduction of tissue necrosis, evidence of granulation tissue and epithelial advancement (Figure 4), and one-week post application continued to yield positive results and wound improvement (Figure 5). At the two-week period, the wound showed significant signs of improvement (Figure 6) and at the three-week mark, NPWTi-d was ceased and standard negative pressure wound therapy (NPWT) dressing applied (Figure 7). The patient was planned to be discharged to a transitional care facility who would not be able to provide ongoing NPWT dressings therefore the patient was stepped down to simple foam dressings and discharged (Figure 8).
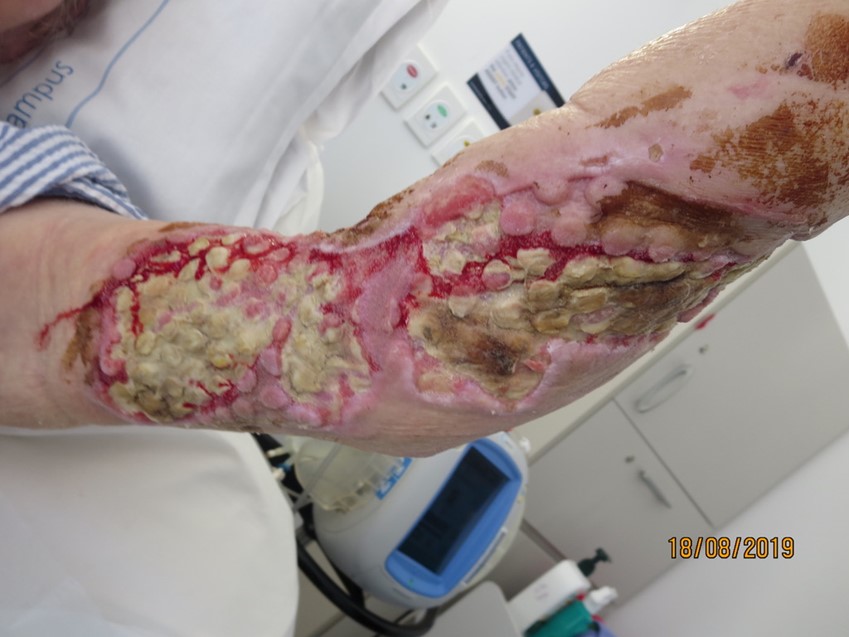
Discussion/Conclusion
This patient had an extensive wound which placed significant stress on his already immunosuppressed body and surgical debridement was not a viable option for this man. Bacterial burden was of great concern, specifically the development of an infection which had the inherent potential to compromise the new hip joint and the patient’s overall health. The efficiency of
NPWTi-d not only expedited debridement, but also managed exudate, promoted granulation and wound contraction and ultimately facilitated the patient’s transition for discharge.