Case Study
Introduction:
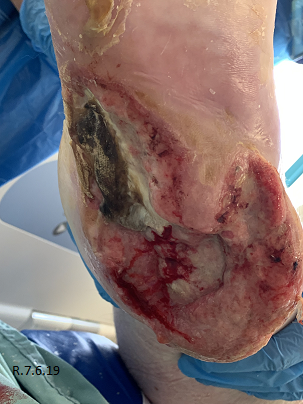
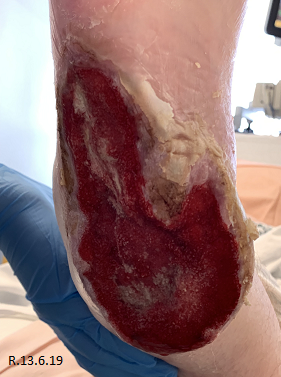
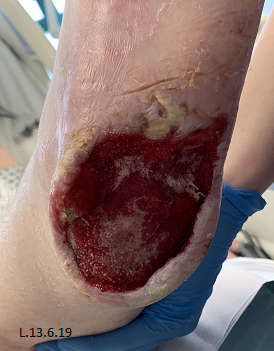
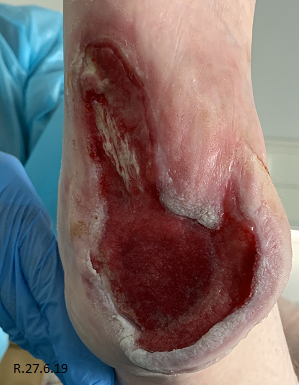
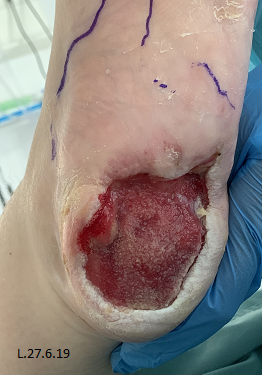
A 34 year old lady (Table 1) admitted from a tertiary hospital with sepsis secondary to stage 4 pressure ulcers to bilateral heels. On examination of feet all soft tissue was displaced off bone posteriorly and medial laterally down to bone with significant wet necrosis (Fig. 1). Bilateral dorsalis pedis pulses were present on doppler.
Table 1.
| Overview of patients characteristics | |
| Gender
Age Weight Residence Diagnosis History |
Female
34 years 120kg Home Sepsis secondary to wet necrosis & osteomyelitis to bilateral heels secondary to stage 4 pressure ulcers. RTA (pedestrian vs car) age 10 Cauda equina 3 years ago, laminectomy and discectomy resulting in peripheral neuropathy and decreased mobility. |
Methods:
Patient was optimised medically. Antibiotic treatment was discussed and commenced as per microbiology and continued for recommended duration. Optimised nutritionally with supplementary naso-gastric feeding, pressure relieving mattress and elevation of heels off bed were initiated to optimise best care. In clinical practice evidence of exposed bone or probing to bone is moderately predictive of osteomyelitis which allows for early commencement of medical treatment with MRI confirming diagnosis (Dinh et. al., 2008). MRI of bilateral ankle/foot was performed to assess extend of injury, findings were highly suspicious of osteomyelitis, the left foot more significant than the right.
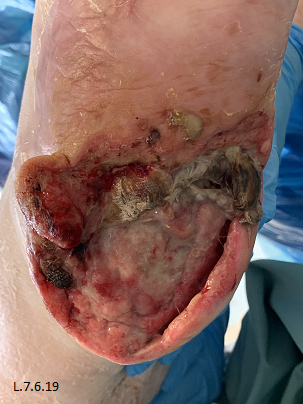
Initial presentation showed devitalised tissue with necrosis which was sharp debrided at the bedside under local anaesthetic 2 days post admission (Fig. 2).
Veraflo™ VAC was applied with prontosan solution as irrigation fluid post debridement. V.A.C Veraflo™ dressing was applied to bilateral heels, prontosan solution was instilled for a 10 minute dwell time, followed by 3.5 hours of continuous negative pressure at 125mmHg. V.A.C. VERAFLO™ dressings were changed twice weekly. After 2 weeks the instillation fluid was changed to sodium chloride (NaCl) for duration of Veraflo™ treatment.
There is limited evidence in the literature to support the use of prontosan over NaCl (Kim et al, 2015), however in view of the presentation of this patient the clinicians favoured the antimicrobial properties of prontosan for initial treatment, Prontosan® wound irrigation solution is a combination of betaine surfactant and polyhexamethylene biguanide (PHMB) antimicrobial which is used to cleanse, rinse and moisturise acute and chronic wounds, prevents the formation of biofilm and can prevent infections and allows for easier dressing changes (BRAUN, 2019).
Results:
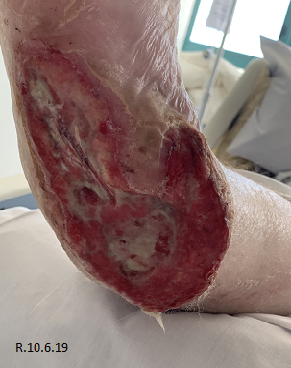
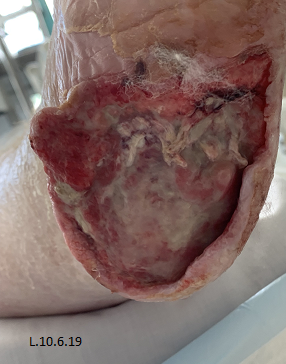
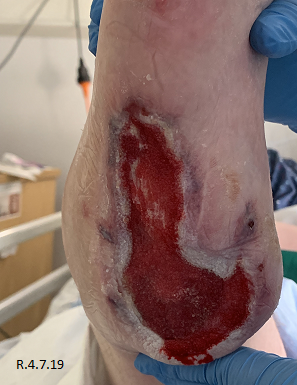
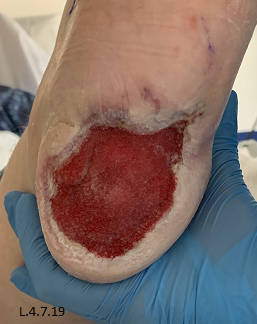
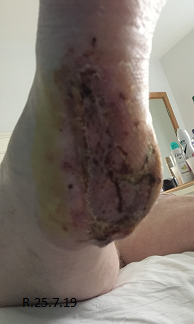
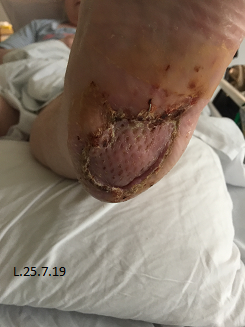
Three days post initial application of Veraflo™ vac with instillation, both wounds showed a marked improvement, with eradication of slough and evidence of healthy granulating tissue (Fig. 3). Both wounds continued to improve over the following weeks, granulating and epithelising in and up from the wound bed resulting in both wounds being suitable for split thickness skin grafting (STSG) which was performed 30 days post commencement of veraflo™ vac and resulted in completely healed wounds post grafting (Table 2) (Fig.4).
Table 2.
| Overview of therapy | |
| Total length of stay Wound swab results Number of days on Veraflo™ Instillation fluid Surgeries Results | 53 days Clostridium species 30 days Prontosan 14 days Sodium chloride 16 days 1-STSG 100% survival of graft Weigh bearing discharged |
Discussion:
Production of granulation tissue to both heels was extraordinarily vigorous considering the extent of the injury and the presence of infection and osteomyelitis, allowing for excellent wound bed preparation for STSG with resultant 100% take and opportunity to commence weigh bearing two weeks post grafting and discharge.
It could be suggested that early intervention and application of the Veraflo™ VAC with instillation optimised this wound bed as an adjuvant to medical systemic management of the underlying infection and condition.
This was a unique case whereby the patient did not have any underlying medical conditions which could have contributed to delayed wound healing however the impressive success achieved in this case highlights the benefit of this treatment modality.
This case study identifies the use of Veraflo™ as a suitable aggressive therapy to optimise the wound bed in as little time as possible allowing for a less traumatic surgical intervention, STSG vs free flap thus potentiating a reduction in length of hospital stay, reduction on impact of hospitalisation both physical and psychological on the patient and a resultant reduction in healthcare costs. Utilising Veraflo™ VAC with instillation as an adjuvant to medical systematic management of the underlying infection and condition has potential positive implications for future use in the treatment of stage 3 and 4 pressure ulcers.
References:
BRAUN (2019) Prontosan®wound irrigation solution. https://www.bbraun.com/en/products/b/prontosan-wound-irrigationsolution.html
Dinh,M.T., Cybele, L.A. & Safdar, N. (2008) Diagnostic accuracy of the physical examination and imaging tests for osteomyelitis underlying diabetic foot ulcers: met-analysis. Clinical Infecious diseases, Vol 47, Is. 4. Pg.519-527
Kim, P.J., Attinger, C.E., Oliver, N., Garwood, C., Evans, K.K., Steinberg, J.S. & Lavery, L.A. (2015) Comparison of outcomes for normal saline and an antiseptic solution for negative-pressure wound therapy with instillation. Plastic and reconstructive surgery, Nov, 657e-664e