Case Study
Abstract Abu Dhabi 2020:
CLINICAL STUDIES INCLUDING CASE SERIES AND CASE REPORTS
Stéphanie Des Rosiers, RN, B.Sc., NSWOCC
CHUM (Montreal University Hospital Center)
Background and Aims
Negative pressure wound therapy with instillation (NPWTi), especially with antimicrobial or antibiotic solutions, has been successful in sternum abscess post cardiac surgery, diabetic foot, necrosis cellulitis, microcirculation deficiency and hernia cure with abdominoplasty, as well as in acute and chronic wounds.
Methods
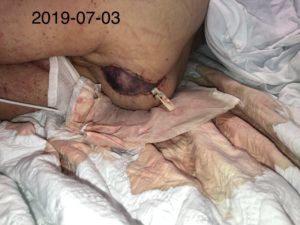
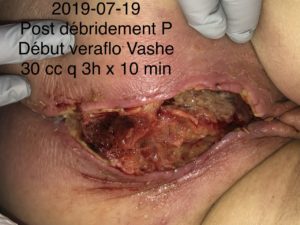
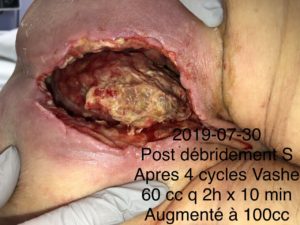
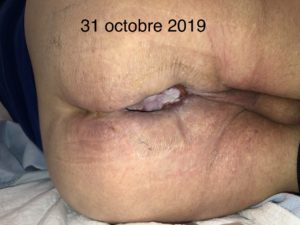
The cohort was patients-individuals (5), men and women, aged from 58 to 82 years old, treated with NPWTi along with saline, antimicrobial and antibiotic solutions. The participants are from Montreal. The assignment to NPWTi of the five participants were based on the wound characteristics. Inclusion criterias were people with necrotic tissues, wound infection, exposed materials or structures, micro circulation deficiency and biofilm.
Results
The participants displayed more granulations and less necrosis in their wounds and avoided amputation, their local infection was controlled and healed quickly. The actual results showed that the wounds of two participants almost closed, one participant had no more necrotic tissues, one had a lot less necrotic tissues while another one avoided amputation for the last four months. In one of the patient, the use of polyhexanide was more efficient than povidone-iodine.
In the litterature, NPWTi with antiseptic prevent bacterial overgrowth and remove exudates, allowing a quicker growth of viable tissue. Polyhexanide 0.1% reduces significantly the bacteria load compared to saline solution 0.9% ou nitrofurazone 0.2%. A review of literature supports polyhexanide and acetic acid as antiseptic substances most suitable for NPWTi in acute and chonic infections and povidone-iodine as prophylaxis in potentially viral contaminated wounds. The studies show that using antibiotic instillation falicitated the reduction of wound bacterial bioburden. There is no specific indication for pressure, the choice of the type of solution, quantity of instillation, time of humidification and frequency. Every decision of these parameters are choosed by clinical judgement, the medical history of the participants and the characteristics of the wound.
Conclusions
We found that NPTi, particularly with antimicrobial or antibiotic solutions, is effective in the context of infections and helps avoid amputation, biofilm, materials or exposed structures, stimulate granulation as well as necrotic tissues for debridement. The treatment demonstrated phenomenal healing time and avoided reinfection of the site. The instillation with vancomycine is something that wasn’t done before, except for one of the five participants. Only a chitosan sponge soaked with vancomycin exists in the literature. Saline and antimicrobial solutions show the same conclusions. More experimental cases need to be done and publish to conclude the choice of the antiseptic solutions.
References
Aguiar, T., Nunes, I., Muralha, N., Ramalho, C & Montenegro, N. (2017). Necrotizing fasciitis after cesarean section: combination of vacuum assisted closure and antiseptic solution instillation as a successful treatment, Acta Obstet Ginecol Port, 11(4), 302-306.
Back, D. A., Scheuermann-Poley & Willy, C. (2013). Recommendations on negative pressure wound therapy with instillation and antimicrobial solutions-when, where and how to use: what does the evidence show?, International Wound Journal,
Dondossola, D., Cavenago, M., Piconi, S., Antonelli, B., Medada, E. & al. (2015). Negative Pressure Wound Treatment of Infections Caused By Extensively Drug-Resistant Gram-Negative Bacteria After Liver Transplantation : Two Case Reports, Transplantation Proceedings, 47, 2145-2149.
Ge, S., Orbay, H., Silverman, R. P. & Rasko, Y. M. (2018). Negative Pressure Wound Therapy with Instillation and Dwell Time in the Surgical Management of Severe Hidradenitis Suppurative, Cureus, 10(9), 1-9.
Gupta, S., Gabriel, A., Lantis, J. & Téot, L. (2016). Clinical recommendations and practical guide for negative pressure wound therapy with instillation, International Wound Journal, 13, 159-174.
Karaca, S. & Afsendiyos, K. (2014). Vacuum-assisted closure (VAC)-Instill® with continuous irrigation for the treatment of Mycoplasma hominis mediastinitis, International Wound Journal, 595-597. doi : 10.1111/iwj.12234.
Ludolph, I., Fried, F. W., Kneppe, K., Arkudas, A., Schmitz, M. & al. (2018). Negative pressure wound treatment with computer-controlled irrigation/instillation decreases bacterial load in contaminated wounds and facilitates wound closure, International Wound Journal, 15, 978-984.
doi : 10.1111/iwj.12958.
Phillips, P. L., Yang, Q. & Schultz, G. S. (2013). The effect of negative pressure wound therapy with periodic instillation using antimicrobial solutions on Pseudomonas aeruginosa biofilm on porcine skin explants, International Wound Journal, 48-55. doi : 10.1111/iwj.12180.
Schultz, G., Phillips, P. L. & Gibson, D. J. (2016). Molecular and cellulor regulators. In Bryant, R. A. & Nix, D. (Eds.), Acute and Chronic Wounds: Current Management Concepts (pp.312-325), Elsevier Health Sciences. Kindle Edition.
Tahir, S., Malone, M., Hu, H., Deva, A. & Vickery, K. (2018). The Effect of Negative Pressure Wound Therapy with and without Instillation on Mature Biofilms In Vitro, 11(811), 1-11. doi : 10.3390/ma11050811.
Tennent, D. J, Shiels, S. M., Jennings, J. A., Haggard, W. O & Wenke, J. C. (2018). Local control of polymicrobial infections via a dual antibiotic delivery system, Journal of Orhtopaedic Surgery and Research, 13(53). https://doi.org/10.1186/s13018-018-0760-y
Wolvos, T. (2013). The Use of Negative Pressure Wound Therapy with an Automated, Volumetric Fluid Administration: An Advancement in Wound Care, Wounds, 25(3), 75-83.